Common Conditions
What is Pulmonary Tuberculosis (TB)?
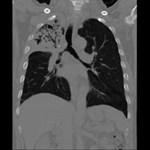
CT scan showing TB of right upper lobe
TB is an infectious disease caused by the organism Mycobacteria tuberculosis. It can be transmitted from person to person. The disease can affect any part of the body such as the brain, bone skin etc. but most often affects the lungs when it is termed pulmonary TB (PTB).
How do I get TB?
TB is transmitted from a person who has active disease and coughing it into the air. Usually, it is someone you spend time with, either a family member or colleague who has active TB. Active TB means someone who may have coughing and abnormal shadows on the chest x-ray and is likely to be coughing out TB germs into the air.
My colleague has active TB, will I get it?
Not everyone who spends time with a patient who has active TB will get active TB. It is estimated that about 15% of people who are close contacts will get infected. This is termed Latent TB Infection ( LTBI). The rest are not infected at all. Of those who have LTBI, only 10 to 15% will eventually develop active TB disease ie. Have cough, chest x-ray changes etc. Close contacts usually refer to family members or colleagues who share the same office.
Do I have Latent TB Infection and what does it mean.
Someone who has been infected with TB but has no symptoms or chest x-ray changes is deemed to have LTBI. Someone with LTBI has a 10 to 15% chance of developing active TB in the future and this usually occurs within 2 years. The only way to tell LTBI is by either doing a skin test ( Mantoux test ) or doing a blood test called ϒ interferon assay. These tests are known by the commercial names of T-spot TB or Quantiferon.
What should be done if I have Latent TB Infection
If you are found to have LTBI AND are a close contact, it is assumed that you are likely to have acquired this from the recent contact. This will be assessed by your doctor. Should this be the case, you may be advised to take 6 or 9 months of isoniazid to reduce the chance of your developing active TB.
If I have active TB, how is it treated?
TB has to be treated with multiple drugs to prevent the emergence of resistance. These have to be taken usually for 6 to 9 moths. The drugs used most often are isoniazid, rifampicin, ethambutol and pyrazinamide. In some centres, patients may be sent for Directly Observed Treatment. This means going for your medications at he polyclinics daily.
What is inactive TB?
After developing active TB, some people actually can keep the disease under control with no treatment. They have chest x-rays with changes suggestive of TB but have no symptoms and are not infectious. The x-rays do not change over time. After a long time, calcium is deposited in the areas affected and the disease is unlikely to become active. However, some patients who have developed this condition recently may benefit from treatment.
What is Multi-drug resistant TB (MDRTB) and extensively drug resistant TB ( XDR-TB)?
MDRTB is TB that is caused by M tuberculosis that is resistant to isoniazid and rifampicin, the 2 most important drugs used in modern TB treatment. MDRTB carries a higher risk of dying and costs significantly more to treat. XDRTB is MDRTB that in addition is also resistant to an injecteble drug and another drug class called quinolones. The vast majority of these cases are caused by poor compliance with treatment.
I feel well 2 weeks after taking my TB medications, why do I need to continue?
The TB germs are very difficult to eradicate. The 6 to 9 months of treatment is to ensure that the patient does not relapse. It is true that most patients will feel reduction in TB symptoms rapidly after taking the medications. However, the TB germs can remain inactive. It is to get rid of these inactive germs that a prolonged treatment course is needed.
